|
1/7/2024 0 Comments Ultrasound screen marker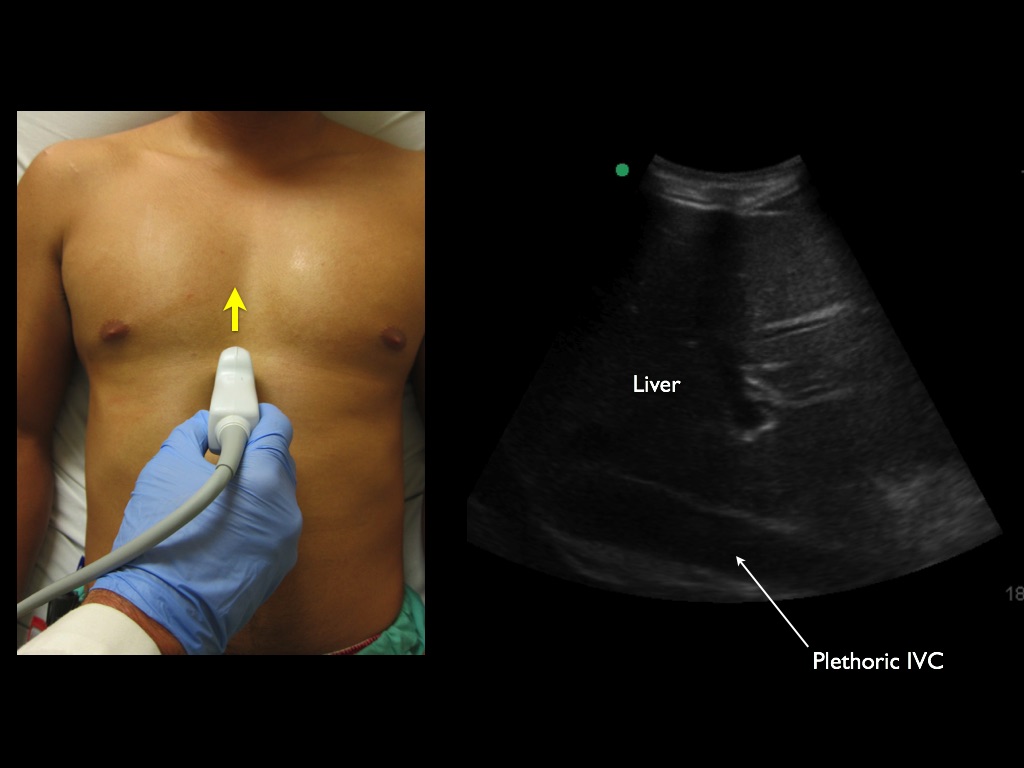
The order of NIPT was not selected as an independent variable predicting the use of IPD. There was no significant association between the numbers of NIPT and IPD with the adjusted ORs between 0.90 and 1.14 (p>0.1). The rate of increase in the NIPT use exceeded the changes in the number of high-risk pregnancies with age ≥35 years, while the number of annual IPD procedures has fluctuated without specific trends. In the cross-sectional assessment, we tested the association between the use of NIPT and IPD using multivariable regression. Longitudinal trends of NIPT order, IPD procedure and the number of patients diagnosed with high-risk pregnancy were descriptively summarised. Cross-sectional utility assessment included 2057 pregnant women. The study consisted of site-level longitudinal analysis and patient-level cross-sectional analysis.Ī total of 5660 new high-risk pregnancies with age ≥35 years were identified for the longitudinal trend analysis. This was a retrospective observational research using healthcare records obtained from an academic healthcare system in the US. 
The objective of this study was to understand the acceptance of NIPT and the utility of NIPT to mitigate concerns about IPD in the US high-risk pregnancy management. In pregnant women with a risk of having fetal congenital disorders, NIPT is anticipated to reduce the needs of invasive prenatal diagnostic test (IPD). Non-invasive prenatal testing (NIPT) is a front-line screening for fatal chromosomal aneuploidy. However, combining the two testing methods yielded the highest detection rate (80% ). We found that ultrasound was more likely to be abnormal than multiple-marker screening tests in fetuses with trisomy 18 (70%) (95% confidence interval 54, 86 versus 43% CI 25, 61). Eleven fetuses (37%) had positive trisomy 18 screens, and two had positive Down syndrome screens, for a total of 13 of 30 (43%) fetuses with positive multiple-marker screening tests. Twenty-one (70%) had abnormalities detected by ultrasound, of which the most common isolated finding was choroid plexus cyst. Ultrasound abnormalities were diagnosed prospectively and were confirmed later by retrospective review of sonographic images.įrom 1988-1997, 30 trisomy 18 fetuses who had comprehensive ultrasounds and multiple-marker testing were identified. A risk of at least 1:190 defined a positive Down syndrome screen. A positive trisomy 18 screen was defined as AFP up to 0.75 multiples of the median (MoM), hCG up to 0.55 MoM, and unconjugated E3 up to 0.60 MoM. To compare detection of trisomy 18 in the second trimester by ultrasound and multiple-marker testing.Ī computerized genetics database was used to identify fetuses of 14-22 weeks' gestation who had comprehensive ultrasound examinations, multiple-marker screening tests (alpha-fetoprotein ), hCG, unconjugated estriol, and trisomy 18 karyotype.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
